Content Outline
Venous Leg Ulcers
21 minute educational videotape
This content outline is provided for informational purposes only. Always consult a qualified health care professional before undergoing any medical treatment. |
|
As the program opens we meet John, a high school teacher who has a venous leg ulcer. John had suffered for years with his leg ulcer, but it is finally healing now because he has learned from his health care professional how to take care of it. We see John wearing a special compression bandage, called an Unna boot. We see him elevating his legs. And we see him walking. John has learned from his health care professional that these simple techniques must be done every day so that his leg ulcer will keep getting better and not come back again. | 
|
Next, the hostess for the program shows us several examples of actual venous leg ulcers. She explains that they usually occur on the inside of the lower leg, often near the ankle. Venous leg ulcers happen to millions of men and women of all ages from all walks of life. We learn that as many as one in four people may have a blood flow problem in their lower legs and could benefit from this information, too. We see pictures of arterial ulcers and diabetic foot ulcers and learn that these types of wounds are treated differently and are not covered in this program. | 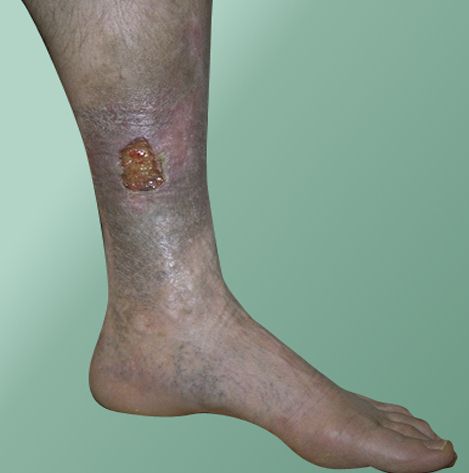
|
Now we learn about the difficult job the heart has in pumping blood up from the lower legs. Without help, high pressure can build up inside the leg veins. Animated graphics show how the calf pump helps to push blood up and out of the leg to keep pressure at a safe level. | 
|
Next we look inside the leg vein to observe how a one-way valve prevents blood from going the wrong direction. We learn that constant high pressure pushing out against the delicate vein walls can stretch the veins out of shape. When that happens the one-way valves do not close well, so blood can go backwards and high pressure can build up. It's called chronic venous insufficiency, or chronic ambulatory venous hypertension. | 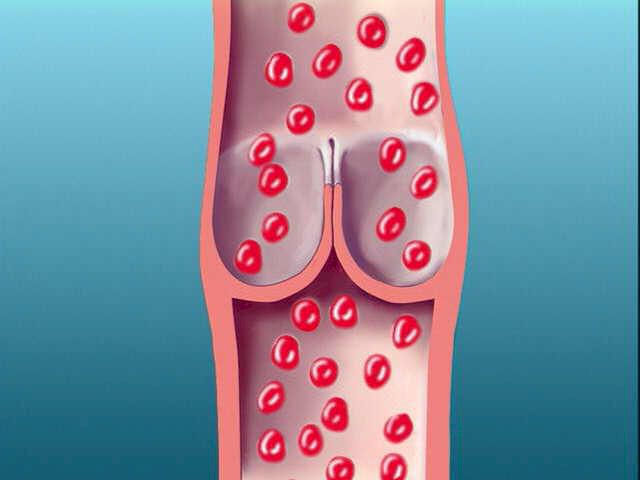
|
We learn that high pressure and damaged veins and valves can happen for many reasons. Often it's a blood clot, called deep vein thrombosis, that causes the damage to the valves and veins. People who have to stand or sit a lot every day in their job are at higher risk.. Pregnancy can be a factor, too. | 
|
The hostess explains that many times, the first sign of high venous pressure in the legs is persistent swelling near the ankles, usually at the end of the day. This is called edema. Varicose veins are a visible sign of increased pressure and damaged veins. Standing may cause a dull aching pain that goes away when the legs are raised. | 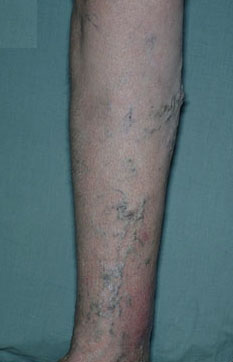
|
Next we see how a venous leg ulcer can get started. With the veins stretched thin from chronic high pressure, we see that blood and fluid can escape through the vein out into the tissue. We watch as the escaped blood turns the skin a brownish color, and makes the leg swell with edema. The hostess explains that the skin is weak and vulnerable now, and just a small bump or scrape could snowball into a serious venous leg ulcer. | 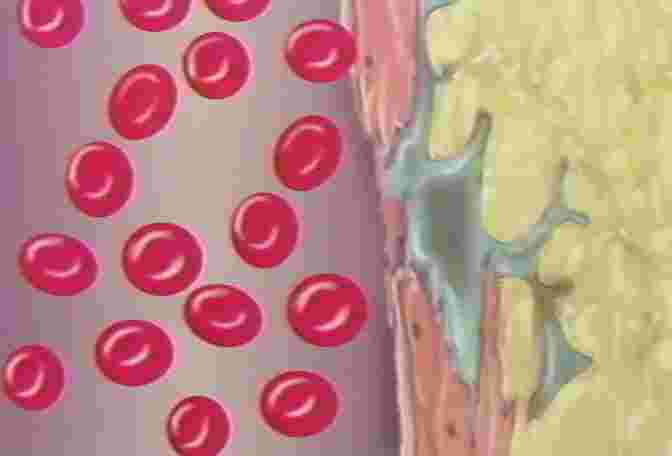
|
We return to John, the high school teacher from the opening of the program. We flash back in time to see John before he had learned how to take care of his leg ulcer. We learn that John had suffered with the leg ulcer for years. He had tried lots of home remedies to make it get better. Sometimes the wound would improve, but it always came back. John was very unhappy. | 
|
Finally, we observe John as he gets some good news from his health care professional. He learns that under a health care professional’s guidance, daily self-care by the patient can help heal most venous leg ulcers and keep many from coming back. Often this includes daily leg compression, elevation of the leg above the heart and some simple calf pump exercises. | 
|
We learn that some patients receive a special diagnostic test called "duplex ultrasound." This painless procedure can provide valuable information about the extent and location of damage. | 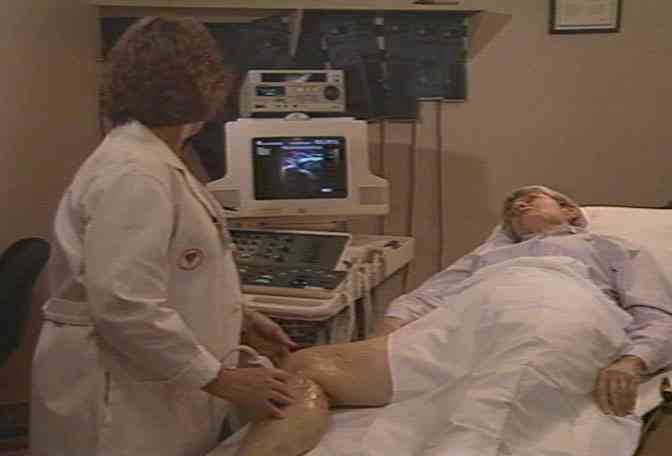 |
Now, we observe John's health care professional as he cleans, inspects and measures John's wound. | 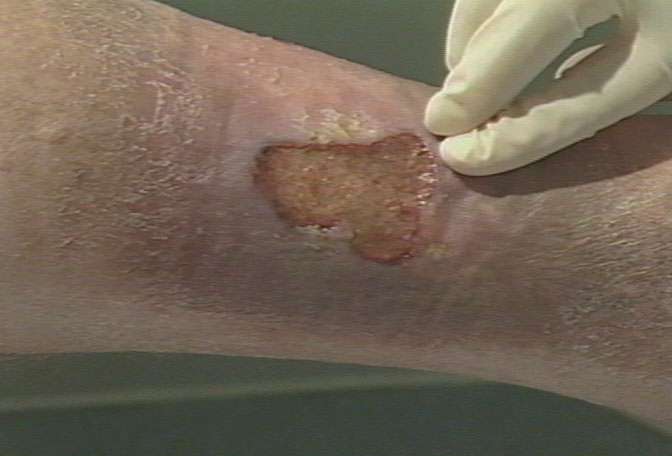 |
Next, John's health care professional applies a layered compression bandage to the wound, starting with a special dressing placed directly against the wound. This is followed by a paste bandage which is wrapped around the leg from the foot up to the calf. Finally, he wraps on a compression bandage. We learn that this type of bandage is very common, but that there are other types of compression bandages from which the health care professional can choose. | 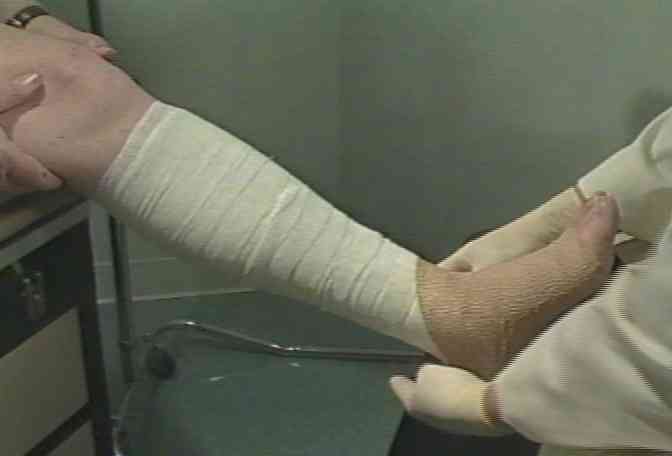
|
At this point the program turns to a description of three self-care activities that are often recommend by health care professionals for their patients with venous leg ulcers or chronic venous insufficiency. We learn that as many as one in four adults may have a blood flow problem in their legs, the early warning signs of which may be pain, swelling or varicose veins. The hostess reminds viewers that anyone with symptoms like these should see a doctor. Such individuals, under the supervision of their health care professional, also may benefit from the self care activities. |  |
The first activity is daily leg compression. We observe individuals using layered compression bandages and compression stockings. We learn that daily leg compression, whether it's from bandages, mechanical pumps or doctor-approved stockings, is essential for wound healing and the prevention of recurrences. Graphics demonstrate the positive effect compression has upon damaged leg veins. | 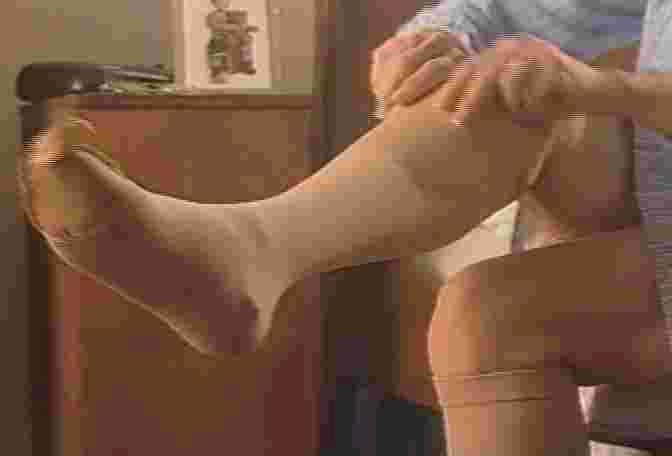 |
The second daily activity is walking and other simple calf pump exercises. We are reminded that the calf pump helps push blood out of the legs. This helps to keep pressure in the leg veins at a safer level. We observe individuals who are unable to take walks as they demonstrate simple calf pump exercises while seated. |  |
The third daily activity is elevating the legs above the heart. The hostess performs a simple demonstration to show how elevation helps to drain blood out of veins. |  |
Finally, the hostess lists six health care practices to help keep legs in good condition, such as wearing comfortable, low-cut shoes and washing legs in mild soap and lukewarm water. | 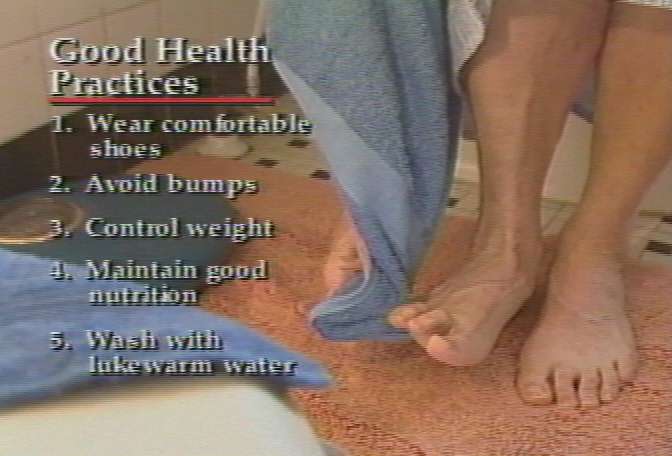 |
The program concludes with a reminder from the hostess that anyone who has a leg ulcer or anyone who thinks they might have a blood flow problem in their legs should talk to a health care professional to find the cause and best treatment. |  |
Varicose Veins - VEIN DISORDERS CENTER - specializing in office surgery (ambulatory phlebectomy) for varicose veins under local anethesia without convalescence and scars
VARICOSE VEINS
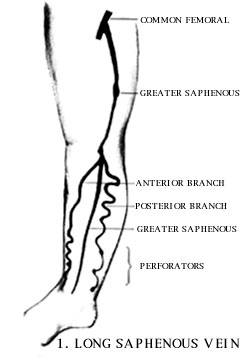
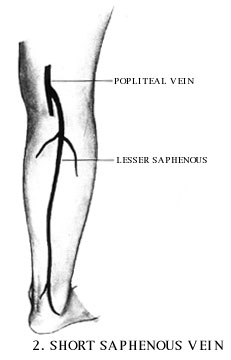
The superficial venous systems of the leg consist of the long and short Saphenous veins.
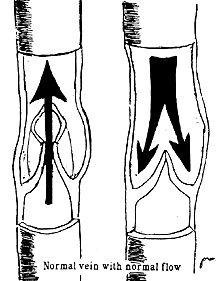
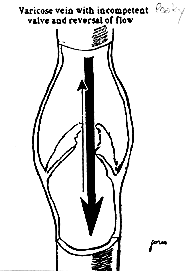
Varicose veins are distended, tortuous / twisted bulging "ropey" superficial veins of the leg that instead of conducting blood upward, back to the heart, conduct blood downward, in a reversed fashion, back to the...foot. This reversed flow pattern is called reflux. As blood accumulates and forms stagnant pools, the veins become visible. All this is possible as the little gates or valves existing in the veins, which ensure a normal unidirectional uphill flow, cannot close properly due to the vein wall distension. This enables gravitation to take over in the upright position, causing the reversed flow pattern. Basically, the existing valves along the vein simply put, leak. As restitution of the normal uphill flow is not possible, a lasting treatment requires control i.e. correction of the reversed flow and removal of the distended varicosities.
TREATMENT MODALITIES
1. CONSERVATIVE (elastic support) TREATMENT. By reducing vein distension, elastic support controls the symptoms of varicose veins such as discomfort, pain and occasional ankle swelling. Elastic stockings also help squeeze the superficial veins and force blood to enter the deep veins and through them go upward, back to the heart. Elastic compression is very useful when definitive treatment cannot be undertaken because of disease, pregnancy or obesity.
2. INJECTION SCLEROTHERAPY for varicose veins should be an appealing therapeutic modality, as it shifts treatment away from the costly hospital care. Unfortunately, however, sclerotherapy in all of its forms, including the much publicized and "fashionable" ultrasound guided injections, cannot control or correct the existing reversed flow patterns and thus should no longer be performed as its results will be only short lived.
WHY DOES INJECTION SCLEROTHERAPY FAIL FOR VARICOSE VEINS? Numerous reports, ours included, have critically evaluated the long term results of this therapeutic modality and have concluded that sclerotherapy carries an unacceptably high (60-100%) 2-5 year failure (recurrence) rate. The reason for that is that sclerotherapy causes a blood clot in the injected vein. This clot will dissipate ("melt") with time and the injected vein will reopen again. This is not difficult to understand if you remember that varicose veins mimic waterfalls that have a top of the hill source of downpour and a bottom of the hill water accumulation or pool(s). So do varicose veins, except that the downpour is blood rather than water. The proximal source of downpour in the case of varicose veins is usually located either at the level of the groin or behind the knee. The varicose branches are the equivalent of the water pools. Siphoning the water from the pools at the bottom of the hill without sound control of the flow (downpour) at the top of the hill will result in rapid refilled pools. Due to the melting clot, sclerotherapy can only temporarily control the proximal source of downpour, therefore, it is easy to understand why just a few months after treatment the reversed flow is reestablished again and the leg varicosities will simply "blossom" in no time.
The handbook of Venous Disorders-Guidelines of American Venous Forum published in January of 1996 by Chapman and Hall Medical clearly states on page 343 that "injection sclerotherapy is contraindicated in varicose veins with communication with a source of reflux (reversed flow)" and on page 399 "experience teaches that sclerotherapy of varicose veins in presence of saphenous reflux (reversed flow) will fail."
We firmly believe, therefore, that it is immoral and unethical to promote and perform a medical procedure with such a high failure rate. If a practitioner still suggests this treatment modality, you are in the wrong hands! We can provide anyone interested with the existing literature on the subject to prove our point.
3. SURGERY is and remains, therefore, the best and the only reliable therapeutic option for varicose veins.
The high ligation, stripping and excision / ligation of varicose veins (shortly known as stripping surgery) is a procedure that was introduced at the turn of the century by three American surgeons (Keller, Mayo and Babcock) It is a very good procedure as it controls the source of downpour and also takes care of the existing varicosities (or "pools" if you prefer). It is still widely used. Unfortunately, however, it is a very traumatic procedure requiring general anesthesia, hospital setting and up to two-three weeks convalescence at home. It is also a very costly procedure too, due to the need for general anesthesia, hospital setting, convalescence and possible loss of income. Basically, the procedure consists of ligating (tying off) the proximal source of the reversed flow (the previously mentioned downpour) which in most of the cases (70-80%) is localized at the groin. This is followed by a "roto-rooter" type procedure called stripping, by which a long wire is threaded into the vein from the groin to the ankle. At this level the vein is secured to a thumb size acorn shaped head attached to the long wire. Traction on the wire at the groin will basically "yank" the whole vein out from the ankle to the groin. The oversized stripper head is responsible for the trauma inflicted to the soft tissues around the vein (with occasional permanent nerve injury) and the long convalescence as well. The remainder of the varicose veins are excised and ligated through usually generous incisions which require several stitches each. The occasional ugly scarring leaves the cosmetic effects of the procedure much to be desired.
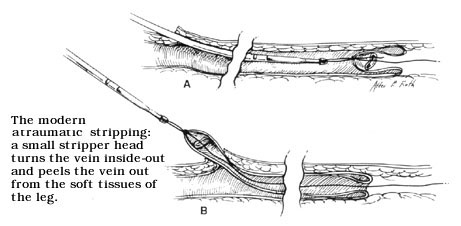
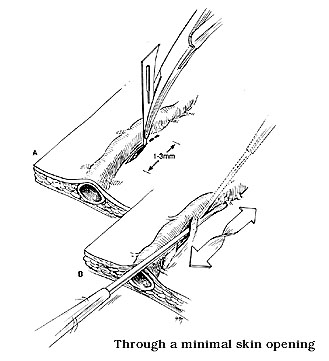
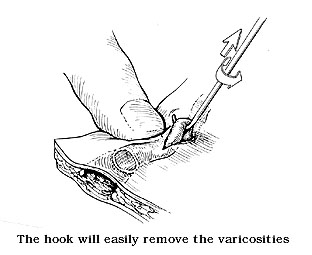
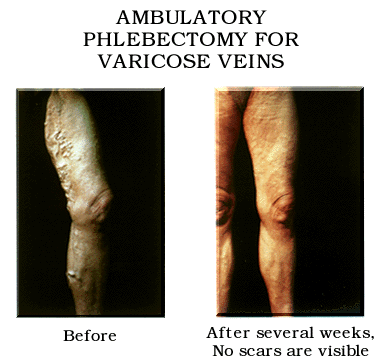
Ambulatory phlebectomy is almost completely a European procedure. Progress in evaluation of the venous system by invasive and non-invasive means produced a better understanding of hemodynamical patterns existing in varicose veins which fueled the dramatic change in the surgical protocol. British surgeons (Rivlin, Negus) first came to the conclusion that stripping from the ankle to groin is not necessary in most cases of varicose veins and that a limited groin to knee stripping is quite sufficient. In some cases it is not even needed at all. At the same time, while still performing the conventional long ankle to groin stripping, a Belgian surgeon (Van der Stricht) reintroduced the more simple, elegant and far less traumatic inverted stripping that was suggested by Keller at the turn of the century. This method was recently further perfected by a Swiss surgeon, a good friend of mine (Oesch). Under this protocol, an atraumatic small headed stripper is turning the vein inside out and is basically peeled out from soft tissues of the leg. No trauma is afflicted to the surrounding soft tissues. Moreover, the introduction of specially designed small hooks, by yet another Swiss physician (Muller) permitted further reduction of operative trauma, as the varicose veins could be now removed through minimal skin openings of 2-3mm that do not require stitches at all. As no scars are visible after 3-4 months,the cosmetic outcome also became much, much improved. We started operating, using this protocol since 1990 and in the past 5 1/2 years we have performed over 900 procedures of the kind with outmost patient and physician satisfaction. We have presented the method in medical meetings and also wrote 7 publications on the subject, some of them with the cooperation of Dr. Yellin from Department of Surgery, University of California Medical School.
We went even further as to perform the procedure in an office setting and under strictly loco-regional anesthesia. That means that 15 minutes after the procedure ( which may last between 1 1/2-2 1/2 hours per leg) the patients is ready to leave the office and drive home and resume his/her normal daily activities, sporting activities included. You will wear, only during the day, a surgical stocking on your leg for one week's time, and you will certainly be able to shower every day. We have not given to a single of our operated patients a certificate of leave of absence as convalescence with this protocol is totally eliminated. In conclusion, ambulatory phlebectomy is a minimally invasive procedure (that is the trend of modern surgery anyhow)and by avoiding general anesthesia, hospital setting and convalescence it is also a very cost efficient procedure as well.